Your Foolproof Guide to Face Masks
Find answers to your questions about face masks: what they are, how to handle them, and how to choose the best one for your needs.

Find answers to your questions about face masks: what they are, how to handle them, and how to choose the best one for your needs.

Published 28 Apr 2026
Article by
6 min read
Face masks are critical protective equipment for COVID-19 prevention. They come in different types offering various levels of protection for every individual. When consistently worn the right way, they help shield the user from the virus. Face masks belong to a comprehensive set of COVID-19 solutions alongside physical distancing, proper handwashing, indoor ventilation, and other measures.
Various face masks offer different levels of protection for its user. The key is to find a well-fitted one that suits your everyday needs, whether you’re a healthcare staff or an office worker.
This section lists three types of face masks and how to use them properly.
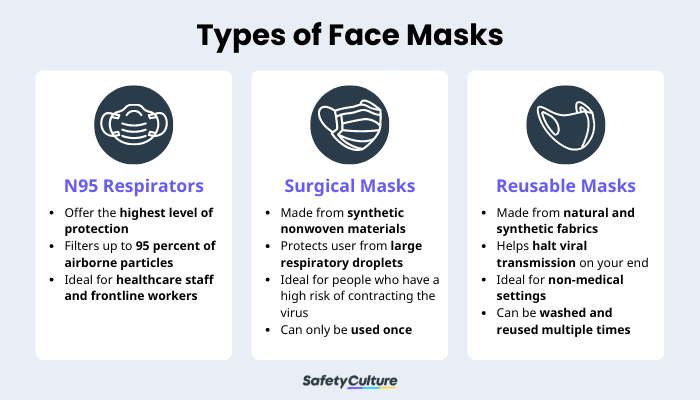
Types of Face Masks
Particulate respirators such as the KN95 and N95 masks offer the highest level of protection for its user. This mask contains specialized filters that trap harmful particles on its surface. It’s tailor-fitted for every user and creates a tight seal to reduce your exposure to airborne particles.
This mask type comes in different grades depending on its filtration rate and approval sources. For example, the US-made N95 masks can filter 95 percent of tiny particles. The National Institute of Occupational Safety and Health (NIOSH) is responsible for regulating its production and use. Other examples include the KN95 masks for China and FFP2 masks for Europe.
Best used for: N95 masks function as Personal Protective Equipment (PPE) for healthcare staff and frontline workers. They also protect caregivers of patients with confirmed or suspected COVID-19 infection.
A surgical mask consists of multiple layers of synthetic non-woven material and filters tucked in the middle. It provides an excellent defense against respiratory droplets. True to its name, this disposable medical mask is commonly used in surgical procedures and must be thrown in the trash bin after using it once.
This mask comes in varying levels of thickness, filtration, and fluid resistance. CDC recommends using it with a cloth mask for added protection.
Best used for: People over the age of 60 or with underlying health conditions can benefit from using disposable masks. It also works for people who are feeling mild symptoms of the virus.
A cloth face mask is the first thing that comes to mind when thinking of reusable face masks. True to its name, this mask is woven from natural and synthetic fabrics. Its multi-layered design helps stop the spread of the virus if you ever contract it.
Best used for: A cloth mask is ideal for everyday use such as grocery shopping and regular office work. Health experts recommend layering it with a surgical face mask for extra protection.
Quality face masks are an essential part of preventing the spread of COVID-19. Various health organizations have released health and safety standards for handling, storing, and making these face covers. This section discusses two pivotal protocols that you should know.
The American Society for Testing and Materials (ASTM) has set the standards for designing effective face masks. The ASTM F3502, endorsed by the NIOSH, outlines six characteristics that manufacturers should follow when making a face mask:
It must cover the user’s mouth and nose.
It should fit comfortably on the sides of the nose and face with no gaps.
It should stay over the mouth and nose during prolonged use.
It should use non-toxic materials that can irritate the skin.
It should be designed for either single or multiple uses.
It should fit or offer sizes for different kinds of individuals.
In the early stages of the pandemic, medical-grade mask supplies were running low because of the sudden increase in demand, panic buying, and hoarding. To resolve this, the US Centers for Disease Control and Prevention (CDC) released a set of strategies to optimize the use of face masks and other PPE supplies during shortages. Healthcare workers and leaders can refer to these methods in case of low supplies.
This guideline includes three capacity stages and their corresponding measures. Healthcare institutes must follow them for an optimal mask distribution. These stages are as follows:
This stage sets the baseline for a healthcare facility’s overall capacity. At the conventional capacity, healthcare centers have an adequate supply of facemasks for their staff. Because of this, healthcare workers can proceed with the standard protocols for handling and discarding masks.
The next step is the contingency capacity. At this level, healthcare facilities experience mask shortages at anticipated rates. By foreseeing the number of face masks needed, these facilities can employ the following temporary measures to mitigate the problem:
Cancel select non-urgent procedures that require the use of face masks as PPE.
Restrict distribution of facemasks only to patients who need them.
Allow an extended use of facemasks as PPE.
If the mask supply can’t meet the predicted rate, this is where the final capacity level comes in. Healthcare facilities must implement optimization measures to combat this crisis:
Cancel all non-urgent appointments that require the use of face masks as PPE.
Wear facemasks beyond recommended shelf life when taking care of patients.
Let healthcare practitioners reuse facemasks for a limited time.
Prioritize the use of facemasks for urgent patient care activities.
With so many face masks available, it may be challenging to choose the best one for your needs. This list will help you narrow down your options for the right mask:
Fitting. It must fit the mouth, nose, and chin comfortably without any gap near the eyes or sides. A snug fit helps prevent droplets from leaking in and out of the mask.
Breathability. Apart from having a good fit, it’s also good to use a mask that you can breathe comfortably in. Some face masks may require you to take breaths with more effort, but they shouldn’t make it harder for you to do so.
Filtration. Face masks come in different filters, depending on the type of mask you use. For example, N95 masks offer the highest level of filtration, making them ideal for high-risk settings such as hospitals. A combination of medical and cloth masks can also filter particles more effectively for healthy individuals.
Material. For cloth face masks, it’s best to use finely woven fabrics that block light when held against a light source. Meanwhile, medical masks typically have synthetic materials with varying layers of protection. Make sure to check the label if it abides by the NIOSH standards.
A range of face masks is available for sale in physical and online stores. Pharmacies, retail shops, and other stores provide them in different materials, filters, and styles for your needs. But if you don’t have the time to go out, you can get high-quality face masks in online shops such as the SafetyCulture Marketplace.
The Marketplace offers N95 masks, disposable face masks, reusable face covers, and other PPEs to keep you safe in the workplace.